Welcome to Crystal Isolate Laser Eye Surgery Sydney
At Crystal Isolate Laser Eye Surgery Sydney, we are dedicated to transforming lives through advanced laser eye surgery. Our experienced team of professionals is committed to providing the highest quality of care, using cutting-edge technology to ensure you achieve the crystal-clear vision you deserve.
OUR LATEST WORK
Explore some of our recent success stories and see the life-changing results we’ve achieved for our patients. Your journey to clearer vision starts here. Contact us today for a personalized consultation.

Simple Home Techniques to Manage Itchy Eyes from Hay-Fever: Sydney Eye Clinic
Get in touch with an eye doctor right away if you suspect anything is wrong with your eyes. One of the most vital functions we have is seeing, thus it’s crucial to protect our eyes. Many tried-and-true home treatments may be relied on to protect and nourish your eyes…

Understanding How Long a Vision Therapy Can Lasts: Sydney Eye Clinic
A vision therapist can help you develop better eye-hand coordination and visual acuity in the same way that a physiotherapist can enhance your physical mobility. A vision therapist can help you develop better eye coordination, response time, and object tracking by developing a personalized therapy plan…
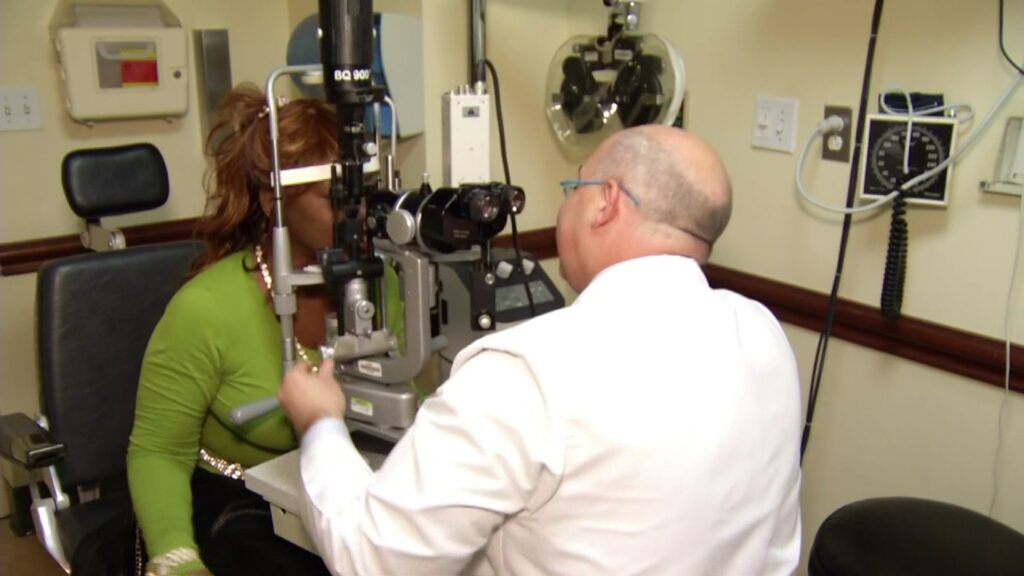
Protecting your Eyes after Undergoing LASIK Eye Surgery
After a successful LASIK eye surgery to rework the shape of the cornea, the patient can enjoy a brighter and sharper vision. However, you also need to learn the best ways to still protect your eyes from any other interference or harmful activity. To ensure the permanent results of your surgery, you should know…
Real Stories, Real Results
Experience the Clarity of Perfect Vision
At Crystal Isolate Laser Eye Surgery Sydney, we offer a range of services tailored to your unique eye care needs and respiratory healthcare with ccollaboration with Air Liquide Healthcare. Our team of experts is dedicated to delivering exceptional results using state-of-the-art techniques. Our main services include:
- Customized Treatment Plans
- Leading-edge Technology
- Compassionate Approach
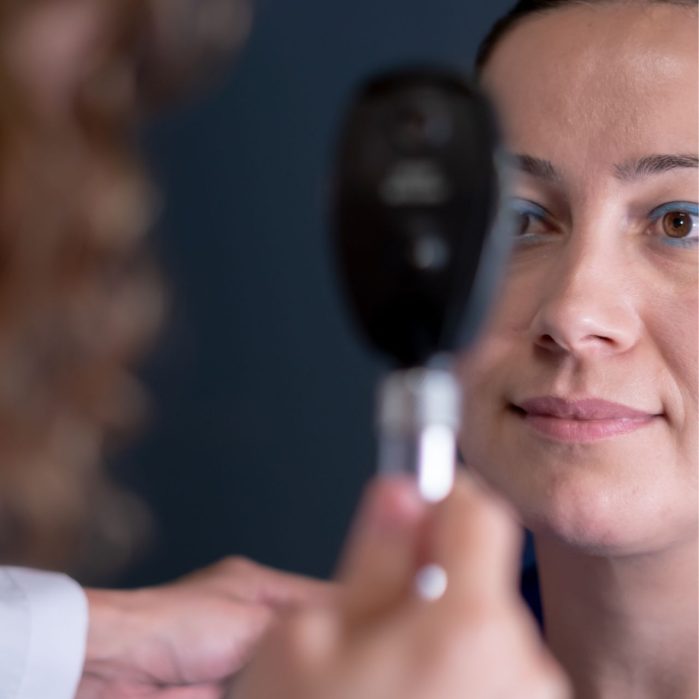




About Our Company
At Crystal Isolate Laser Eye Surgery Sydney, we are dedicated to helping you achieve your best vision. With a reputation for excellence and a team of skilled professionals, we are your trusted partner in eye care.
- Cataract Surgery
- LASIK Eye Surgery
- Laser Eye Surgery
- Retinal Treatments
Our Professional Approach
"I can't believe the difference after my cataract surgery at Crystal Isolate Laser Eye Surgery Sydney. The world is so much clearer now!"
"LASIK surgery was life-changing for me. Crystal Isolate's team made the process smooth, and I'm enjoying a glasses-free life!"
"I had laser eye surgery at Crystal Isolate and I'm amazed by the results. The procedure was quick and painless, and my vision is better than ever."

Jesse Hewlett
- 304-592-6057

Sebastian Henn
- 949-884-6539

Ryan MacCarthy
- 970-612-7053