Understanding Chronic Pain; The Causes, Differences and Management
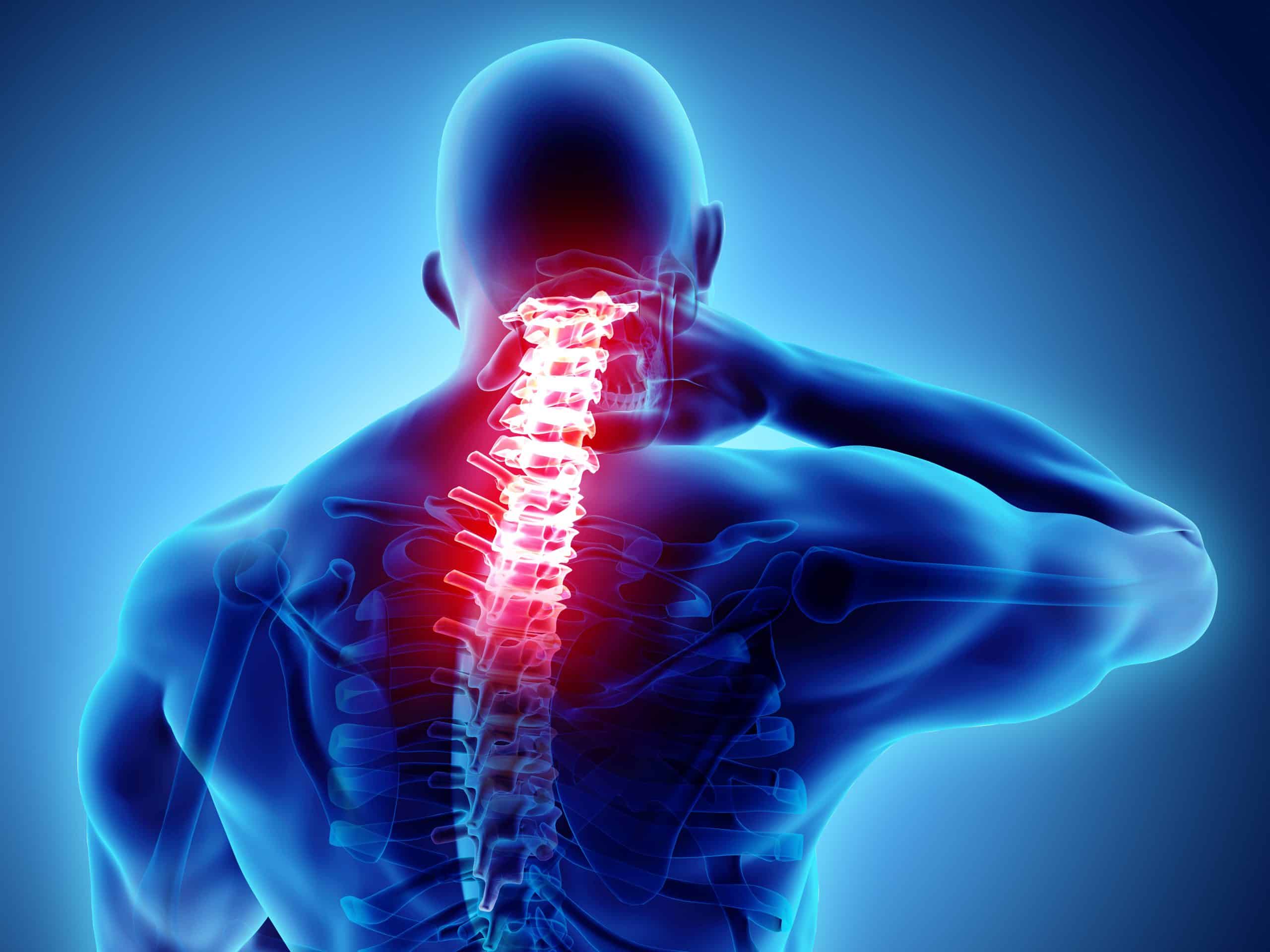
The sensation caused by different chronic pain syndromes is affected by a variety of variables. To better understand the complexities of this prevalent illness, this article may be of great use to you. Below is a list of model on chronic pain symptoms.
Disruption of normal tissue function. In this case the initial source of chronic pain syndrome is just the damaged or injured tissue, because of the injury to the tissues, the nervous system then receives stimuli (the pain signal) which then transcend to other parts of the body. The phrase “nociceptive input” describes this as well.
Feeling of discomfort or pain. In this simplified model, chronic pain perception happens in the brain after a nerve signal has travelled from the periphery to the brain. Pain perception takes place in the brain, while nociception happens at the site of damage.
Related: What You Need to Know About Chronic Pain Syndrome?
Thoughts. Higher brain centres process the incoming pain sensation signal and the surrounding circumstances in order to form a cognition, or idea. In either case, these mental processes significantly alter how one interprets the incoming chronic pain signal. For example, sore muscles and joints are considered “good pain” after a strong workout, but “bad pain” when caused by a medical disease like fibromyalgia.
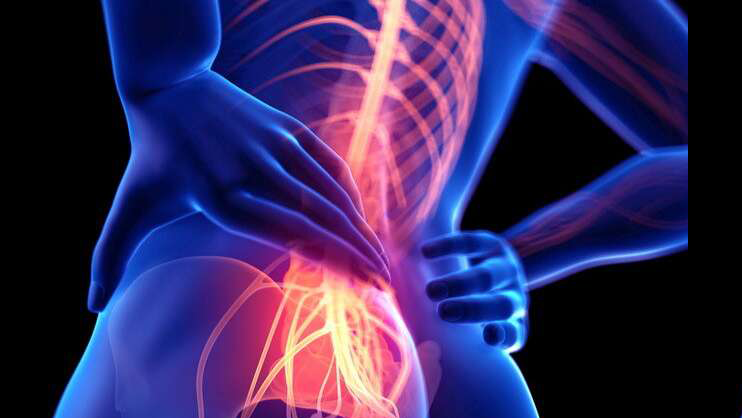
Emotions. An individual’s reaction to contemplating the pain is the emotional component of pain. Fear, melancholy, and worry are just some of the feelings that may surface if you think the source of your discomfort is a life-threatening condition, such a tumour. On the other hand, if you don’t take the pain seriously, you won’t react strongly to it.
Suffering. Despite their scientific and conceptual differences, the terms “suffering” and “pain” are sometimes used interchangeably. Some types of pain, such as those associated with a shattered bone, might occur without constituting true suffering. In contrast, while a broken bone may produce immediate discomfort, the suffering associated with bone pain caused by a tumour is likely to be far more severe because of the underlying the pain. The emotional component of chronic pain symptoms is intrinsically linked to the experience of suffering.
Distressing actions. Pain behaviors are actions taken by persons in response to physical discomfort. Typical outward signs of pain include complaining about it, making a grimace, limping, moving slowly, and using pain medication. In the pain system paradigm, pain behaviors are a result of all the other components (tissue damage, pain sensation, thoughts, emotions, and suffering). The ways in which people react to pain depend not only on the nature of the suffering itself, but also on their upbringing, social environment, and other factors. It’s interesting to note that environmental factors, such as how other people react, might have an effect on chronic pain-related behaviours.
The Transition from Acute Pain to Chronic Pain
Understanding the distinction between acute and chronic pain is essential for both the doctor and the patient. The pain experienced by someone experiencing acute pain is a sign of damaged or diseased tissues, and the intensity of the pain experienced by someone experiencing acute pain is proportional to the extent of the damage. When an injury has healed completely, the pain associated with it usually goes away. If you have a herniated disc, for instance, and you relieve the pressure on the nerve, the severe pain will go away. Because of this, the goal of medical treatment for acute pain is to alleviate the underlying condition that is triggering the pain.
However, there is no protective or other biological purpose for Chronic pain syndrome. Here, we refer solely to the chronic pain subtype.

The Development of Chronic Pain
While the progression of acute pain may be traced back to a clear set of causes and effects, the development of chronic pain can take many different forms. In addition, not all persistent pain is chronic pain, and there is substantial heterogeneity even among patients with the same diseases. Sometimes the pain from a major ailment is little, and sometimes the agony from a minor condition is excruciating.
Treatments for chronic pain might have varying degrees of success from one individual to the next. One person may get relief from pain caused by a herniated disc with a certain drug or injection, whereas another person may find no relief at all.
Factors unrelated to tissue damage and injury become increasingly relevant as pain progresses from the acute to the chronic stage. One factor is that chronic pain signals in, in the absence of actual tissue injury. Stress, sadness, and a reduction in fitness as a result of inactivity can all play a role.
Treating Chronic Pain Medically
The medical Specialisation of pain management has expanded to include chronic pain as a distinct area, being recognised as a fundamental issue in its own right, rather than only a symptom or sign of a more serious underlying condition.
Doctors that specialise in chronic pain management are able to alleviate a wide variety of painful conditions. A multidisciplinary team is typically used to manage pain in cases of chronic pain, since this allows for all components of the pain to be addressed simultaneously. Consequences, areas such as tissue damage (if present), mental and emotional states, the experience of pain, suffering, and the surrounding environment, all figure prominently here as they did in the original model. Physicians with a background knowledge in psychologists and physiatry or anaesthesiology with expertise in clinical health psychology make up the bulk of this therapy modality. Precisely, physiatrists diagnose and treat disorders in the musculoskeletal system (the muscles, nerves, and bones) that cause mobility issues. Doctors who specialise in physical medicine and rehabilitation are commonly referred to as “physiatrists.” Methods are tailored to the person, and they aim to alleviate pain in all of its psychological and physiological manifestations.
Spinal cord and peripheral nerve stimulation, as well as x-ray-guided injections, are just a few of the interventional and minimally invasive techniques used by anaesthesiologists to alleviate chronic pain.
Psychologists in clinical practise who have a focus on pain treatment frequently collaborate with the attending physician. A psychologist investigates mental and emotional states in addition to pain and environmental factors.
Everyone with chronic pain issue desire nothing more than to have this condition leave them total. For effective chronic pain treatment, if you are experiencing it, you should book a consultation session with specialists at Chronic Therapy.